What Is Mortons Neuroma
May 29, 2017 Comments Off on What Is Mortons Neuroma
Overview
.jpg) Also known as Morton’s Interdigital Neuroma, Morton’s Metatarsalgia, Morton’s Neuralgia, Plantar Neuroma, Intermetatarsal Neuroma) What is a Morton’s neuroma? Morton’s neuroma is a condition characterized by localized swelling of the nerve and soft tissue located between two of the long bones of the foot (metatarsals – figure 1), which can result in pain, pins and needles, or numbness in the forefoot or toes.
Also known as Morton’s Interdigital Neuroma, Morton’s Metatarsalgia, Morton’s Neuralgia, Plantar Neuroma, Intermetatarsal Neuroma) What is a Morton’s neuroma? Morton’s neuroma is a condition characterized by localized swelling of the nerve and soft tissue located between two of the long bones of the foot (metatarsals – figure 1), which can result in pain, pins and needles, or numbness in the forefoot or toes.
Causes
A Morton’s neuroma commonly occurs due to repetitive weight bearing activity (such as walking or running) particularly when combined with tight fitting shoes or excessive pronation of the feet (i.e. “flat-feet”). The condition is also more common in patients with an unstable forefoot allowing excessive movement between the metatarsal bones. A Morton’s neuroma can also occur due to certain foot deformities, trauma to the foot, or the presence of a ganglion or inflamed bursa in the region which may place compressive forces on the nerve.
Symptoms
A Morton’s neuroma usually causes burning pain, numbness or tingling at the base of the third, fourth or second toes. Pain also can spread from the ball of the foot out to the tips of the toes. In some cases, there also is the sensation of a lump, a fold of sock or a “hot pebble” between the toes. Typically, the pain of a Morton’s neuroma is relieved temporarily by taking off your shoes, flexing your toes and rubbing your feet. Symptoms may be aggravated by standing for prolonged periods or by wearing high heels or shoes with a narrow toe box.
Diagnosis
The doctor will ask about your symptoms and medical history. A physical exam will be done. Initial diagnosis of Morton’s neuroma is based on your description of the type and location of pain and discomfort in the foot. The diagnosis will be confirmed by a physical exam of the foot, including checking for mechanical abnormalities in the foot, squeezing the side of the foot, which will usually cause pain when Morton’s neuroma is present. Examination of your shoes to check for excess wear in parts of the shoe, check to see whether the shoes are too tight. Imaging tests evaluate the foot and surrounding structures. This may be done with X-ray, MRI scan, Ultrasound. Injections of local anesthetic can also be used for diagnosis.
Non Surgical Treatment
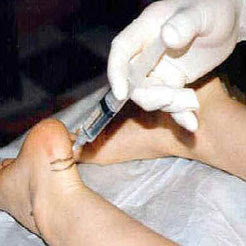
Treatment for Morton?s Neuroma usually begins conservatively, with a change in lifestyle choices. People suffering from the condition may find pain relief by reducing activity levels, changing footwear, using orthopedic supports, reducing weight. Medications are also available to help relieve the pain of Morton?s Neuroma. Over-the-counter medications are sometimes very helpful in reducing pain and inflammation. Your health care provider can also provide you with anesthetic or corticosteroid injections. These help to numb the area affected by the neuroma, and reduce inflammation.
Surgical Treatment
If these non-surgical measures do not work, surgery is sometimes needed. Surgery normally involves a small incision (cut) being made on either the top, or the sole, of the foot between the affected toes. Usually, the surgeon will then either create more space around the affected nerve (known as nerve decompression) or will cut out (resect) the affected nerve. If the nerve is resected, there will be some permanent numbness of the skin between the affected toes. This does not usually cause any problems. You will usually have to wear a special shoe for a short time after surgery until the wound has healed and normal footwear can be used again. Surgery is usually successful. However, as with any surgical operation, there is a risk of complications. For example, after this operation a small number of people can develop a wound infection. Another complication may be long-term thickening of the skin (callus formation) on the sole of the foot (known as plantar keratosis). This may require treatment by a specialist in care of the feet (chiropody).
What May Cause Posterior Calcaneal Spur
September 29, 2015 Comments Off on What May Cause Posterior Calcaneal Spur

Overview
A calcaneal spur (or heel spur) is a small osteophyte (bone spur) located on the calcaneus (heel bone). Calcaneal spurs are typically detected by a radiological examination (X-ray). When a foot bone is exposed to constant stress, calcium deposits build up on the bottom of the heel bone. Generally, this has no effect on a person’s daily life. However, repeated damage can cause these deposits to pile up on each other,causing a spur-shaped deformity, called a calcaneal (or heel) spur. Obese people, flatfooted people, and women who constantly wear high-heeled shoes are most susceptible to heel spurs. An inferior calcaneal spur is located on the inferior aspect of the calcaneus and is typically a response to plantar fasciitis over a period, but may also be associated with ankylosing spondylitis (typically in children). A posterior calcaneal spur develops on the back of the heel at the insertion of the Achilles tendon. An inferior calcaneal spur consists of a calcification of the calcaneus, which lies superior to the plantar fascia at the insertion of the plantar fascia. A posterior calcaneal spur is often large and palpable through the skin and may need to be removed as part of the treatment of insertional Achilles tendonitis. These are also generally visible to the naked eye.
Causes
Everyone can be affected by heel spurs, however, certain groups of people have an increased risk. For example, Plantar Fasciitis is a common running injury. People who walk a lot are much more likely to have heel spurs or people who play golf or play tennis. Over-weight people are also more at risk for heel bone spurs as our feet are not designed to carry around extra weight. As a result the ligaments under the foot are placed under constant stress, which inevitably will lead to foot problems.

Symptoms
With heel spurs, people often talk about a dull ache which is felt most of the time with episodes of a sharp pain in the center of the heel or on the inside margin of the heel. Often the pain is worse on first rising in the morning and after rest and is aggravated by prolonged weight bearing and thin-soled shoes.
Diagnosis
The proper diagnosis of a heel spur often requires an X-ray. To make this process as convenient for his patients as possible, most clinics have an on-site digital X-ray and diagnostic ultrasound machines. This can make it unnecessary for patients to visit diagnostic imaging centers, allowing patients to receive more expedient treatment.
Non Surgical Treatment
Heel spurs are considered a self-limited condition, which means that by making small alterations in your lifestyle and regular routines you can often control the condition. The goal is to relieve pain, reduce friction and transfer pressure from your sensitive foot areas. By eliminating the cause of the heel spur and plantar fasciitis (i.e. better shoes, orthotics to fix your gait, losing weight) will help reduce the pressure put on your fascia and heel and can reduce the inflammation caused by your heel spur. Failure to see improvements after conservative treatments may make surgery your only option.
Surgical Treatment
Surgery involves releasing a part of the plantar fascia from its insertion in the heel bone, as well as removing the spur. Many times during the procedure, pinched nerves (neuromas), adding to the pain, are found and removed. Often, an inflamed sac of fluid call an accessory or adventitious bursa is found under the heel spur, and it is removed as well. Postoperative recovery is usually a slipper cast and minimal weight bearing for a period of 3-4 weeks. On some occasions, a removable short-leg walking boot is used or a below knee cast applied.
Ways To Treat Calcaneal Spur
September 26, 2015 Comments Off on Ways To Treat Calcaneal Spur

Overview
Heel spurs occur in at least half the people who have plantar fasciitis, a painful condition involving the thick tissue that runs between your heel bone and your toes. In the past, doctors often performed surgery to remove heel spurs, believing them to be the cause of the pain associated with plantar fasciitis. In treating plantar fasciitis now, doctors rely more on ice, arch supports, physical therapy and pain medications, and surgery is rarely performed.
Causes
Bone spurs can form anywhere in the feet in response to tight ligaments, repetitive stress injuries (typically from sports), obesity, even poorly fitting shoes. For instance, when the plantar fascia on the bottom of the foot pulls repeatedly on the heel, the ligament becomes inflamed, causing plantar fasciitis. As the bone tries to mend itself, a bone spur forms on the bottom of the heel, typically referred to as a heel spur. This is a common source of heel pain.
Symptoms
Most of the time heel spurs present as pain in the region surrounding the spur, which typically increases in intensity after prolonged periods of rest. Patients may not be able to bear weight on the afflicted heel comfortably. Running, walking, or lifting heavy weight may exacerbate the issue.
Diagnosis
The proper diagnosis of a heel spur often requires an X-ray. To make this process as convenient for his patients as possible, most clinics have an on-site digital X-ray and diagnostic ultrasound machines. This can make it unnecessary for patients to visit diagnostic imaging centers, allowing patients to receive more expedient treatment.
Non Surgical Treatment
Treatment of Heel Spurs is the same as treatment of plantar fasciitis. To arrive at an accurate diagnosis, our foot and ankle Chartered Physiotherapists will obtain your medical history and examine your foot. Throughout this process the physio will rule out all the possible causes for your heel pain other than plantar fasciitis. The following treatment may be used. Orthotics/Insoles. Inflammation reduction. Mobilisation. Taping and Strapping. Rest.
Surgical Treatment
In a small number of cases (usually less than 5 percent), patients may not experience relief after trying the recommendations listed above. It is important that conservative treatments (such as those listed above) be performed for AT LEAST a year before considering surgery. Time is important in curing the pain from heel spurs, and insufficient treatment before surgery may subject you to potential complications from the procedure. If these treatments fail, your doctor may consider an operation to loosen the plantar fascia, called a plantar fascia release.
Prevention
You can prevent heel spurs by wearing well-fitting shoes with shock-absorbent soles, rigid shanks, and supportive heel counters; choosing appropriate shoes for each physical activity; warming up and doing stretching exercises before each activity; and pacing yourself during the activities. Avoid wearing shoes with excessive wear on the heels and soles. If you are overweight, losing weight may also help prevent heel spurs.
Healthy Treatment For Bursitis Feet
August 23, 2015 Comments Off on Healthy Treatment For Bursitis Feet
Overview
Retrocalcaneal bursitis is closely related to Haglund?s Deformity (or ?pump bumps?). If you have a bony enlargement on the back of the heel that rubs the Achilles tendon, it can cause the formation of a bursa (small fluid filled sack). It usually happens in athletes as shoes rub against the heel. The bursa can aggravated by the stitching of a heel counter in the shoe as well. It can make wearing shoes and exercising difficult. Another term used for this condition is ?pump bump? because it can frequently occur with wearing high heels as well. ?Retro-” means behind and ?calcaneus? means heel bone. So this is precisely where the bursitis (inflammation of the bursa) develops. Once it begins and you develop bursitis between the heel bone and the Achilles tendon, it can become even more painful. When most people first notice retrocalcaneal bursitis, it is because the skin, bursa and other soft tissues at the back of the heel gets irritated as the knot of bone rubs against the heel counter in shoes. The back of the shoes create friction and pressure that aggravate the bony enlargement and pinches the bursa while you walk.
Causes
The retrocalcaneal bursa can become inflamed as the result of another condition, such as damage to the Achilles tendon, osteoarthritis, rheumatoid arthritis, gout, and pseudogout. In these instances, the treatment for bursitis must accompany treatment for the underlying condition. Septic retrocalcaneal bursitis, which is caused by an infection, is uncommon. Infection can reach the bursa through a cut, puncture, a blister, or even an insect bite. It is possible to have septic bursitis without an obvious opening. In these cases the superficial wound may have healed quickly, but still allowed bacteria into the bursa.
Symptoms
Symptoms of bursitis include pain in the heel, especially with walking, running, or when the area is touched. The skin over the back of the heel may be red and warm, and the pain may be worse with attempted toe rise (standing on tippy-toes).
Diagnosis
Your doctor will check for bursitis by asking questions about your past health and recent activities and by examining the area. If your symptoms are severe or get worse even after treatment, you may need other tests. Your doctor may drain fluid from the bursa through a needle (aspiration) and test it for infection. Or you may need X-rays, an MRI, or an ultrasound.
Non Surgical Treatment
The most important part of treating bursitis is resting your Achilles tendon while the bursa heals. Resting your ankle as much as possible may decrease swelling and keep the bursitis from getting worse. When the pain decreases, begin normal, slow movements. Ice causes blood vessels to constrict (get small) which helps decrease inflammation (swelling, pain, and redness). Put crushed ice in a plastic bag or use a bag of frozen corn or peas. Cover it with a towel. Put this on your heel for 15 to 20 minutes, three to four times each day. Do not sleep on the ice pack because you can get frostbite. After two or three days, you may try using heat to decrease pain and stiffness. Use a hot water bottle, heating pad, whirlpool or warm, moist compress. To make a compress, dip a clean washcloth in warm water. Wring out the extra water and put it on your heel for 15 to 20 minutes, three to four times each day. Your caregiver may tell you to switch between treating your heel with ice packs and heat treatments. Follow the caregiver’s directions carefully when doing these treatments.
Surgical Treatment
Surgery is rarely need to treat most of these conditions. A patient with a soft tissue rheumatic syndrome may need surgery, however, if problems persist and other treatment methods do not help symptoms.
Hammer Toe Deformity
June 26, 2015 Comments Off on Hammer Toe Deformity
 Overview
Overview
What are hammertoes, mallet toes and claw toes? Often the words are used interchangeably to mean an abnormally contracted toe like the drawing above. Technically speaking, a “hammertoes” is the name for a toe that is contracted at the first toe joint. If it’s contracted at the second toe joint it is called a “mallet toe”. IIf a toe is contracted at both toe joints, it is called a “claw toe”. Each of these conditions can be quite uncomfortable and are cosmetically unappealing.
Causes
Wearing shoes that squeeze the toes or high heels that jam the toes into the front of the shoe. Other causes or factors in the development of hammertoes can include an injury such as badly stubbing your toe, arthritis and nerve and muscle damage from diseases such as diabetes. And, hammertoes tend to run in families, although it is more likely the faulty foot mechanics that lead to hammertoes that are inherited, not the hammertoes themselves. Hammertoe generally affect the smaller toes of the foot, especially the second toe, which for many people is the longest toe. It’s uncommon for the big toe to be bent this way.
 Symptoms
Symptoms
The most obvious symptoms of this injury will be the the middle toe joint is permanently bent at an angle. In the beginning movement may still be possible but as time passes and the injury worsens the toe will be locked in place and possible require hammer toe correction surgery to fix. Another key indicator of hammer toe is that a lump or corn will form on top of the toe. The toe joint will be painful and walking can cause severe discomfort. Occasionally a callus may form on the sole of the injured foot. If you see any of these symptoms together or have been enduring pain for some time, seeing a podiatrist should be your next step.
Diagnosis
Although hammertoes are readily apparent, to arrive at a diagnosis the foot and ankle surgeon will obtain a thorough history of your symptoms and examine your foot. During the physical examination, the doctor may attempt to reproduce your symptoms by manipulating your foot and will study the contractures of the toes. In addition, the foot and ankle surgeon may take x-rays to determine the degree of the deformities and assess any changes that may have occurred.
Non Surgical Treatment
Conservative treatment is limited to accommodation, not correction, of the deformity, though some patients find the relief they can get from these options to be more than enough to put off or even avoid surgery. These include better Footwear. Shoe gear with a wider toe box and higher volume causes less friction to the toes. Toe Braces and Strapping. Some toe braces and strapping techniques take some pressure off the toes during gait. Custom molded orthotics can redistribute the forces through the tendons that control the toe, lessening the pain and extent of the deformity.The calluses on the toe and the ball of the foot can be shaved occasionally to reduce some pain and pressure, although they will return due to the constant deformity.
Surgical Treatment
Bone-mending procedures realign the contracted toe by removing the entire deviated small joints of the toe (again, not at the ball of the foot). This allows for the Hammer toe buckled joint to be positioned flat and the bone ends to mend together. Often surgical hardware (fixation) is necessary to keep the bones steady during healing. Hardware options can involve a buried implant inside the toe, or a temporary wire that is removed at a later date. Medical terminology for this procedure is called a proximal interphalangeal joint arthrodesis (fusion), or a distal interphalangeal joint arthrodesis (fusion), with the former being performed in a high majority of cases.
 Prevention
Prevention
elect and wear the right shoe for specific activities (such as running shoes for running). Alternate shoes. Don’t wear the same pair of shoes every day. Avoid walking barefoot, which increases the risk for injury and infection. At the beach or when wearing sandals, always use sunblock on your feet, as you would on the rest of your body. Be cautious when using home remedies for foot ailments. Self-treatment can often turn a minor problem into a major one. It is critical that people with diabetes see a podiatric physician at least once a year for a checkup. People with diabetes, poor circulation, or heart problems should not treat their own feet, including toenails, because they are more prone to infection.
Hammer Toe Treatments
June 25, 2015 Comments Off on Hammer Toe Treatments
 Overview
Overview
Hammer toe can affect any of the toes on the foot except the big toe, though the most common toe to suffer is the second one. While the smallest toe can be affected, the condition causes the toe to twist out to the side rather than to curl forward. Hammertoe is not very discriminating; it may appear on all four toes of the foot or on only one toe, depending on the cause.
Causes
Hammertoe Hammer toe has three main culprits: tight shoes, trauma, and nerve injuries or disorders. When toes are crowded in shoes that are too tight and narrow, they are unable to rest flat, and this curled toe position may become permanent even when you aren’t wearing shoes due to the tendons of the toe permanently tightening. When the tendons are held in one position for too long, the muscles tighten and eventually become unable to stretch back out. A similar situation may result when tendons are injured due to trauma, such as a stubbed, jammed, or broken toe.
 Symptoms
Symptoms
Hammer toes can cause problems with walking and lead to other foot problems, such as blisters, calluses, and sores. Pain is caused by constant friction over the top of the toe?s main joint. It may be difficult to fit into some shoe gear due to the extra space required for the deformed toe. In many cases there will be pain on the ball of the foot over the metatarsals along with callus formation. This is due to the toes not functioning properly, failing to properly touch the ground during the gait cycle. The ball of the foot then takes the brunt of the ground forces, which causes chronic pain.
Diagnosis
Most health care professionals can diagnose hammertoe simply by examining your toes and feet. X-rays of the feet are not needed to diagnose hammertoe, but they may be useful to look for signs of some types of arthritis (such as rheumatoid arthritis) or other disorders that can cause hammertoe.
Non Surgical Treatment
Your podiatrist may recommend conservative treatment techniques for your hammertoes based on your foot structure, which will likely involve removing any thick, painful skin, padding your painful area, and recommending for you shoes that give your curled toes adequate room. Conservative care strategies for this health purpose may also involve the use of Correct Toes, our toe straightening and toe spacing device.
Surgical Treatment
Surgery is used when other types of treatment fail to relieve symptoms or for advanced cases of hammertoe. There are several types of surgeries to treat hammertoe. A small piece of bone may be removed from the joint (arthroplasty). The toe joint may be fused to straighten it (arthrodesis). Surgical hardware, such as a pin, may be used to hold the bones in place while they heal. Other types of surgery involve removing skin (wedging) or correcting muscles and tendons to balance the joint.
 Prevention
Prevention
Although the feet naturally change over time, and abnormalities like hammertoes may be hereditary for some patients, steps may be taken to prevent their development in the first place. Just as better fitting shoes are a treatment, they are also a preventative measure for hammertoes. In addition, your podiatrist may suggest orthotics to improve the biomechanics of your feet in an effort to prevent the development of hammertoes or other abnormalities. Calf stretching and other exercises may also be used to reverse or treat muscle imbalances that could eventually lead to hammertoe development.
Hallux Valgus Deformity Symptoms
June 12, 2015 Comments Off on Hallux Valgus Deformity Symptoms
Overview

The term “hallux valgus” or “hallux abducto-valgus” are the most commonly used medical terms associated with a bunion anomaly, where “hallux” refers to the great toe, “valgus” refers to the abnormal angulation of the great toe commonly associated with bunion anomalies, and “abductus/-o” refers to the abnormal drifting or inward leaning of the great toe towards the second toe, which is also commonly associated with bunions. It is important to state that “hallux abducto” refers to the motion the great toe moves away from the body’s midline. Deformities of the lower extremity are usually named in accordance to the body’s midline, or the line bisecting the body longitudinally into two halves. In more severe cases, the hallux continuing in the abductus fashion eventually either overlaps or underlaps subsequent lesser (small) toes especially the second (adjacent toe).
Causes
With prolonged wearing of constraining footwear your toes will adapt to the new position and lead to the deformity we know as a foot bunion. Footwear is not the only cause of a bunion. Injuries to the foot can also be a factor in developing a bunion. Poor foot arch control leading to flat feet or foot overpronation does make you biomechanically susceptible to foot bunions. A family history of bunions also increases your likelihood of developing bunions. Many people who have a bunion have a combination of factors that makes them susceptible to having this condition. For example, if you are a women over the age of forty with a family history of bunions, and often wear high-heeled shoes, you would be considered highly likely to develop a bunion.
SymptomsPatients with bunions will often display pain over the prominent bump on the inside of their forefoot (the medial eminence?). However, they may also have pain under the ball of the foot (under the area near the base of the second toe). Symptoms can vary in severity from none at all to severe discomfort aggravated by standing and walking. There is no direct correlation between the size of the bunion and the patient?s symptoms. Some patients with severe bunion deformities have minimal symptoms, while patients with mild bunion deformities may have significant symptoms. Symptoms are often exacerbated by restrictive shoe wear, particularly shoes with a narrow toe box or an uncomfortable, stiff, restraining upper.
Diagnosis
Although bunions are usually obvious from the pain and unusual shape of the toe, further investigation is often advisable. Your doctor will usually send you for X-rays to determine the extent of the deformity. Blood tests may be advised to see if some type of arthritis could be causing the pain. Based on this evaluation, your doctor can determine whether you need orthopaedic shoes, medication, surgery or other treatment.
Non Surgical Treatment
When the deformity is mild, treatment is usually not necessary. However, changing shoes to ones that have little or no heel, and are wider in the toe area (toe box) will be more comfortable and may help to prevent worsening of the bunion deformity. If the bunion starts to become painful, other measures may help. Bunions can cause pain in several different areas. The medial eminence may be painful, the entire first toe joint may hurt, or there may be pain underneath some or all of the forefoot (the ball of the foot). Pain over the medial eminence is the most common problem that affects bunion patients. A ?toe spacer? can be placed between the first and second toes and can provide some pain relief as it straightens out the bunion slightly. Pads placed over the medial eminence itself are hard to keep in place and rarely help to relieve pain. Pain underneath the first toe or lesser toes can be relieved by pads placed in the shoes in precise areas. The pads help to take pressure off the prominent areas on the bottom of the foot. Generalized measures to relieve bunion pain, such as physical therapy or foot stretching exercises, have not been shown to be helpful. Orthotics are often prescribed, but are also rarely helpful in relieving pain over the bunion, but may help with pain felt under the ball of the foot.

Surgical Treatment
If non-surgical treatments have failed to relieve your bunion pain, or when the pain is interfering with your daily activities, contact the Dallas bunion surgery specialists at North Texas Foot & Ankle to discuss surgical options. There are a several ways to perform bunion surgery. The best procedure for one person is not necessarily the best for another. Some procedures allow you to walk much sooner, reducing the need for crutches. Depending on your foot type, the procedure can have a greater risk for return of the bunion deformity. Other procedures may require you to be on crutches for a few weeks – but could offer a better result in the long-term. Learn more about the different types of bunion surgery.
What Are The Most Obvious Chief Causes Of Overpronation Of The Foot
May 29, 2015 Comments Off on What Are The Most Obvious Chief Causes Of Overpronation Of The Foot
Overview
Pronation is a normal motion which occurs after heel strike during walking. As the foot moves towards toe off, the foot naturally should move from an outside path towards the midline of the body stopping at neutral in ideal conditions. Overpronation is the foot?s motion past neutral and moving excessively toward the bodies midline. Overpronation can be caused by a number of factors including internal rotation of the femur or thigh bone, internal torsion of the tibia or shin bone, being genu valgum or ?knock kneed?, as well as fixed deformities of the ankle and forefoot. The overpronating foot is often hypermobile meaning it has excessive range of motion in the foot joints.
Causes
Over-pronation may happen because the tissue that attaches to your foot bones is loose. You may be born with this problem or it may result from injuries or overuse, like from too much running.
Symptoms
If you overpronate, your symptoms may include discomfort in the arch and sole of foot, your foot may appear to turn outward at the ankle, your shoes wear down faster on the medial (inner) side of your shoes. Pain in ankle, shins, knees, or hips, especially when walking or running are classic symptoms of overpronation. Overpronation can lead to additional problems with your feet, ankles, and knees. Runners in particular find that overpronation can lead to shin splints, tarsal tunnel syndrome, plantar fasciitis, compartment syndrome, achilles tendonitis, bunions or hallux valgus, patello-femoral pain syndrome, heel spurs, metatarsalgia.
Diagnosis
Bunions, calluses and crooked toes may indicate alignment problems. So, it is important to ascertain the condition of a client’s toes. Check the big toe to determine if the first joint of the toe is swollen, has a callus or bunion, and/or looks as though it abducts (i.e., hallux valgus) rather than pointing straight ahead. Also, look to see if the lesser toes seem to “curl up” (i.e., the person has hammer or claw toes). This may be indicative of damage to, or inflexibility of the plantar fascia caused by excessive flattening of the foot.
Non Surgical Treatment
Over-Pronation can be treated conservatively (non-surgical treatments) with over-the-counter orthotics. These orthotics should be designed with appropriate arch support and medial rearfoot posting to prevent the over-pronation. Footwear should also be examined to ensure there is a proper fit. Footwear with a firm heel counter is often recommended for extra support and stability. Improperly fitting footwear can lead to additional foot problems.
Prevention
With every step we take, we place at least half of our body weight on each foot (as we walk faster, or run, we can exert more than twice our body weight on each foot). As this amount of weight is applied to each foot there is a significant shock passed on to our body. Custom-made orthotics will absorb some of this shock, helping to protect our feet, ankles, knees, hips, and lower back.
Severs Disease The Facts
May 20, 2015 Comments Off on Severs Disease The Facts
Overview
The calcaneal apophysis is a growth center where the Achilles tendon and the plantar fascia attach to the heel. It first appears in children aged 7 to 8 years. By ages 12 to 14 years the growth center matures and fuses to the heel bone. Injuries can occur from excessive tension on the Achilles tendon and the plantar fascia, or from direct impact on the heel. Excessive stress on this growth center can cause irritation of the heel, also called Sever?s disease.
Causes
Severs disease is often associated with a rapid growth spurt. As the bones get longer, the muscles and tendons become tighter as they cannot keep up with the bone growth. The point at which the achilles tendon attaches to the heel becomes inflamed and the bone starts to crumble (a lot like osgood schlatters disease of the knee). Tight calf muscles may contribute as the range of motion at the ankle is reduced resulting in more strain on the achilles tendon. Sever’s disease is the second most common injury of this type which is known as an apophysitis.
Symptoms
Unilateral or bilateral heel pain. Heel pain during physical exercise, especially activities that require running or jumping or are high impact. Pain is often worse after exercise. A tender swelling or bulge on the heel that is painful on touch. Limping. Calf muscle stiffness first thing in the morning.
Diagnosis
Sever’s disease is diagnosed based on a doctor?s physical examination of the lower leg, ankle, and foot. If the diagnosis is in question, the doctor may order X-rays or an MRI to determine if there are other injuries that may be causing the heel pain.
Non Surgical Treatment
The immediate goal of treatment is pain relief. Because symptoms generally worsen with activity, the main treatment for Sever’s disease is rest, which helps to relieve pressure on the heel bone, decreasing swelling and reducing pain. As directed by the doctor, a child should cut down on or avoid all activities that cause pain until all symptoms are gone, especially running barefoot or on hard surfaces because hard impact on the feet can worsen pain and inflammation. The child might be able to do things that do not put pressure on the heel, such as swimming and biking, but check with a doctor first.
Prevention
Can Calcaneal Apophysitis Be Prevented? The chances of a child developing heel pain can be reduced by avoiding obesity. Choosing well-constructed, supportive shoes that are appropriate for the child?s activity. Avoiding or limiting wearing of cleated athletic shoes. Avoiding activity beyond a child?s ability.
What Can Cause Heel Ache
March 30, 2015 Comments Off on What Can Cause Heel Ache
Overview
Heel pain is often a symptom caused by one of two conditions: Plantar Fasciitis or Achilles Tendonitis. Most commonly, heel pain experienced at the bottom of the heel is caused by plantar fasciitis. Heel Pain may become so severe for some that just putting weight on their feet first thing in the morning is excruciating. Walking or running may feel completely out of the question.
Causes
The two major causes of heel pain are plantar fasciitis and achilles tendinitis. The easiest way to figure out which one is causing your pain is by location. Generally speaking, if the pain is under your heel bone it is likely plantar fasciitis. If the pain is found at the back of the heel, in the achilles or toward the base of the achilles (the long cord that extends from your calf to your heel bone), then it is likely achilles tendinitis.
Symptoms
Symptoms of plantar fasciitis vary, but the classic symptom is pain after rest–when you first get out of bed in the morning, or when you get up after sitting down for a while during the day. The pain usually diminishes after a few minutes of walking, sometimes even disappearing, but the pain is commonly felt again the longer you’re on the foot. Fasciitis can be aggravated by shoes that lack appropriate support, especially in the arch area, and by the chronic irritation of long-periods of standing, especially on concrete, by being overweight. It doesn’t help that fascia doesn’t heal particularly quickly because it has relatively poor circulation (which is why it’s white in colour).
Diagnosis
A podiatrist (doctor who specializes in the evaluation and treatment of foot diseases) will carry out a physical examination, and ask pertinent questions about the pain. The doctor will also ask the patient how much walking and standing the patient does, what type of footwear is worn, and details of the his/her medical history. Often this is enough to make a diagnosis. Sometimes further diagnostic tests are needed, such as blood tests and imaging scans.
Non Surgical Treatment
Recommended treatments, heel Spurs: cushioning for the heel is of little value. Your chiropodist/podiatrist may initially apply padding and strapping to alter the direction of stretch of the ligament. This is often successful at reducing the tenderness in the short term. Your chiropodist/podiatrist may suggest a course of deep heat therapy to stimulate the healing processes, allowing damage to respond and heal faster. In the long term, your chiropodist/podiatrist may prescribe special insoles (orthoses) to help the feet to function more effectively, thereby reducing strain on the ligaments and making any recurrence less likely. If pain from heel spurs continues, you may be referred to your GP who can prescribe an oral non-steroidal anti-inflammatory. Alternatively, localised hydrocortisone injection treatment may be given by your GP or an appropriate chiropodist/podiatrist. If pain persists, surgery may be considered. Heel Bursitis: in most cases, attention to the cause of any rubbing, and appropriate padding and strapping by your chiropodist/podiatrist will allow the inflammation to settle. If infection is present, your chiropodist/podiatrist will refer you to your GP for antibiotics. Heel Bumps: adjustments to footwear is often enough to make them comfortable. A leather heel counter and wearing boots may help. However, if pain persists, surgery may be necessary.
Surgical Treatment
When a diagnosis of plantar fasciitis is made early, most patients respond to conservative treatment and don?t require surgical intervention. Often, when there is a secondary diagnosis contributing to your pain, such as an entrapped nerve, and you are non-responsive to conservative care, surgery may be considered. Dr. Talarico will discuss all options and which approach would be the most beneficial for your condition.
Prevention

You can try to avoid the things that cause heel pain to start avoid becoming overweight, where your job allows, minimise the shock to your feet from constant pounding on hard surfaces, reduce the shocks on your heel by choosing footwear with some padding or shock-absorbing material in the heel, if you have high-arched feet or flat feet a moulded insole in your shoe may reduce the stresses on your feet, if you have an injury to your ankle or foot, make sure you exercise afterwards to get back as much movement as possible to reduce the stresses on your foot and your heel in particular, If you start to get heel pain, doing the above things may enable the natural healing process to get underway and the pain to improve.
You must be logged in to post a comment.